Articles
- Page Path
- HOME > Restor Dent Endod > Volume 51(2); 2026 > Article
- Review Article Effectiveness of silver diamine fluoride in managing hypersensitivity of molar-incisor hypomineralization affected molars: a scoping review
-
Vo Truong Nhu Ngoc1
 , Do Trong Hieu2
, Do Trong Hieu2 , Tran Anh Tuan1,*
, Tran Anh Tuan1,* , Vo Nhat Minh1
, Vo Nhat Minh1 , Trinh Khanh Linh1
, Trinh Khanh Linh1
-
Restor Dent Endod 2026;51(2):e19.
DOI: https://doi.org/10.5395/rde.2026.51.e19
Published online: April 13, 2026
1School of Dentistry, Hanoi Medical University, Hanoi, Vietnam
2Faculty of Dentistry, University of Medicine and Pharmacy, Vietnam National University, Hanoi, Vietnam
- *Correspondence to Tran Anh Tuan, DDS School of Dentistry, Hanoi Medical University, No. 1 Ton That Tung Street, Kim Lien Ward, Dong Da District, Hanoi 100000, Vietnam Email: trananhtuan09302@gmail.com
© 2026 The Korean Academy of Conservative Dentistry
This is an Open-Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/4.0) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
- 1,649 Views
- 180 Download
Abstract
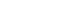
- This study aimed to evaluate the efficacy of dentinal hypersensitivity treatment with silver diamine fluoride (SDF) in molar-incisor hypomineralization (MIH)-affected molars. This scoping review was designed and structured according to the guidelines of the Preferred Reporting Items for Systematic Reviews and Meta-Analyses and its extension for scoping reviews. A search strategy was conducted across PubMed, The Cochrane Library, ScienceDirect, and Google Scholar to identify articles related to the topic. Two authors screened titles, abstracts, and full texts for review. Five studies met the eligibility criteria, comprising four randomized controlled trials and one case report, with sample sizes ranging from four to 200 participants. All included studies reported improvements in clinical outcomes, including reduced hypersensitivity following SDF application, as indicated by lower Schiff cold air sensitivity scale scores. SDF is a promising treatment strategy for reducing hypersensitivity in MIH-affected molars; however, further research using SDF alone is needed to evaluate its exact effectiveness.
INTRODUCTION
METHODS
RESULTS
1. Demographics of participants
2. Study locations and treatment methods
3. Follow-up periods
DISCUSSION
CONCLUSIONS
-
CONFLICT OF INTEREST
No potential conflict of interest relevant to this article was reported.
-
FUNDING/SUPPORT
The authors have no financial relationships relevant to this article to disclose.
-
DISCLOSURE OF GENERATIVE AI IN SCIENTIFIC WRITING
During the preparation of this work, the authors used ChatGPT ver. 5.3 (OpenAI, San Francisco, CA, USA) in order to improve the readability and language of the manuscript during the writing process. After using this tool, the authors reviewed and edited the content as needed and take full responsibility for the content of the published article.
-
AUTHOR CONTRIBUTIONS
Conceptualization, Methodology: all authors. Data curation, Formal analysis, Investigation: Tuan TA, Minh VN , Linh TK. Writing - original draft: Ngoc VTN, Hieu DT, Tuan TA, Minh VN. Writing - review & editing: all authors. All authors read and approved the final manuscript.
-
DATA SHARING STATEMENT
The data supporting this article can be made available by the corresponding author upon request.
| No. | Study | Year | Research location | Research type | Sample (people) | Sample (molar) | Sex | Age (yr) | Research strategy | Tooth severity | Follow- up interval |
|---|---|---|---|---|---|---|---|---|---|---|---|
| 1 | Khan [24] | 2022 | India | Case report | 1 | 4 | Male | 8 | Evaluate the effect of SDF + stainless steel in reducing sensitivity on MIH-affected molars. | Severe | 3 mo |
| 2 | Ballikaya et al. [23] | 2022 | Türkiye | RCTs | 48 | 112 | Female, 30/male, 18 | 8.8 ± 1.58 | Evaluate and compare the effect of SDF and SMART sealants for the treatment of initial carious lesions of permanent molars affected by MIH. | NA | 1 mo, 6 mo, and 12 mo |
| 3 | Erbas Unverdi et al. [17] | 2024 | Türkiye | RCTs | 48 | 112 | Female, 30/male, 18 | 8.8 ± 1.58 | Assess the clinical outcomes of utilizing SDF + KI treatment and SMART/SDF + KI + GIC | NA | 12 mo, 18 mo, 24 mo, and 36 mo |
| 4 | Saad et al. [22] | 2024 | Egypt | RCTs | 28 | 56 | Female, 20/male, 8 | 6–10 | Compare SMART vs the conventional restoration and fluoride varnish application on moderate to severe MIH teeth | Moderate–severe | 1 wk, 6 mo, and 12 mo |
| 5 | Al-Nerabieah et al. [21] | 2024 | Syria | RCTs | 100 | 200 | NA | 6–9 | Compare the efficacy of SDF and CPP-ACPFV in preventing caries development, enamel breakdown, and sensitivity on molars affected by MIH in children. | Mild | 3 mo, 6 mo, 9 mo, and 12 mo |
CPP-ACPFV, casein phosphopeptide-amorphous calcium phosphate fluoride varnish; GIC, glass ionomer cement; KI, potassium iodide; MIH, molar incisor hypomineralization; NA, not applicable; RCT, randomized clinical trial; SDF, silver diamine fluoride; SMART, silver-modified atraumatic restorative treatment.
| No. | Study | Treatment result | |||||
|---|---|---|---|---|---|---|---|
| SDF | SDF + KI | SMART/SDF + KI + GIC | SDF + stainless steel | CCP-ACPFV | Conventional restoration and fluoride varnish | ||
| 1 | Khan [24] | NA | NA | NA | SCASS scores deduce | NA | NA |
| 2 | Ballikaya et al. [23] | SCASS scores deduce | NA | SCASS scores deduce | NA | NA | NA |
| - Baseline: 1.77 ± 0.83 | - Baseline: 1.77 ± 0.83 | ||||||
| - 12th month: 0.15 ± 0.38 | - 12th month: 0.08 ± 0.28 | ||||||
| 3 | Erbas Unverdi et al. [17] | NA | SCASS scores deduce | SCASS scores deduce | NA | NA | NA |
| - SCASS scores = 0 (at the 18-month and beyond evaluations) | - SCASS scores = 0 (at the 18-month and beyond evaluations) | ||||||
| 4 | Saad et al. [22] | NA | NA | SCASS scores deduce | NA | NA | SCASS scores deduce |
| - Baseline: +MOD: 1.5/+ SEV: 3 | - Baseline: +MOD: 1.5/+SEV: 3 | ||||||
| - 12th month: +MOD: 0/+SEV: 0 | - 12th month: +MOD: 0/+SEV: 0 | ||||||
| 5 | Al-Nerabieah et al. [21] | SCASS scores deduce | NA | NA | NA | SCASS scores deduce | NA |
CPP-ACPFV, casein phosphopeptide-amorphous calcium phosphate fluoride varnish; GIC, glass ionomer cement; KI, potassium iodide; MIH, molar incisor hypomineralization; MOD, moderate hypomineralized molar severity; NA, not applicable; SCASS, Schiff cold air sensitivity scale; SDF, silver diamine fluoride; SEV, severe hypomineralized molar severity; SMART, silver-modified atraumatic restorative treatment.
| No. | Study | Treatment result | |||||
|---|---|---|---|---|---|---|---|
| SDF | SDF + KI | SMART/SDF+KI+GIC | SDF + stainless steel | CCP-ACPFV | Conventional restoration and fluoride varnish | ||
| 1 | Khan [24] | NA | NA | NA | NA | NA | NA |
| 2 | Ballikaya et al. [23] | - No dental caries presented | NA | - No dental caries presented | NA | NA | NA |
| - Retention rate: NA | - Retention rate: 88.7% | ||||||
| 3 | Erbas Unverdi et al. [17] | NA | - The caries preventive effect was 100%, 67.9%, and 65.4% at 12, 24, and 36 months, respectively | - The caries preventive effect was 100%, 97.6%, and 94.7% at 12, 24, and 36 months, respectively | NA | NA | NA |
| - Retention rate: NA | - Retention rate: 88.7%, 73.1%, and 66.6% at 12, 24, and 36 months, respectively | ||||||
| 4 | Saad et al. [22] | NA | NA | - Caries prevention: NA | NA | NA | - Caries prevention: NA |
| - Restoration integrity | - Restoration integrity | ||||||
| +6th month: MOD: 1, SEV: 1 | +6th month: MOD: 1, SEV: 1 | ||||||
| +12th month: MOD: 1, SEV: 1 | +12th month: MOD: 1, SEV: 1 | ||||||
| 5 | Al-Nerabieah et al. [21] | - Caries rate was 11%, 15%, 21%, and 23% at 3, 6, 9, and 12 months, respectively | NA | NA | NA | - Caries rate was 33%, 39%, 44%, and 49% at 3, 6, 9, and 12 months, respectively | NA |
| - Retention rate: NA | - Retention rate: NA | ||||||
CPP-ACPFV, casein phosphopeptide-amorphous calcium phosphate fluoride varnish; GIC, glass ionomer cement; KI, potassium iodide; MIH, molar incisor hypomineralization; MOD, moderate hypomineralized molar severity; NA, not applicable; SDF, silver diamine fluoride; SEV, severe hypomineralized molar severity; SMART, silver-modified atraumatic restorative treatment.
- 1. Weerheijm KL. Molar incisor hypomineralisation (MIH). Eur J Paediatr Dent 2003;4:114-120.PubMed
- 2. Kirthiga M, Poornima P, Praveen R, Gayathri P, Manju M, Priya M. Prevalence and severity of molar incisor hypomineralization in children aged 11-16 years of a city in Karnataka, Davangere. J Indian Soc Pedod Prev Dent 2015;33:213-217.ArticlePubMed
- 3. Weerheijm KL, Duggal M, Mejàre I, Papagiannoulis L, Koch G, Martens LC, et al. Judgement criteria for molar incisor hypomineralisation (MIH) in epidemiologic studies: a summary of the European meeting on MIH held in Athens, 2003. Eur J Paediatr Dent 2003;4:110-113.PubMed
- 4. Almuallem Z, Busuttil-Naudi A. Molar incisor hypomineralisation (MIH): an overview. Br Dent J 2018;225:601-609.Article
- 5. Fearne J, Anderson P, Davis GR. 3D X-ray microscopic study of the extent of variations in enamel density in first permanent molars with idiopathic enamel hypomineralisation. Br Dent J 2004;196:634-638.ArticlePubMedPDF
- 6. Raposo F, de Carvalho Rodrigues AC, Lia ÉN, Leal SC. Prevalence of hypersensitivity in teeth affected by molar-incisor hypomineralization (MIH). Caries Res 2019;53:424-430.ArticlePDF
- 7. Lygidakis NA, Garot E, Somani C, Taylor GD, Rouas P, Wong FS. Best clinical practice guidance for clinicians dealing with children presenting with molar-incisor-hypomineralisation (MIH): an updated European Academy of Paediatric Dentistry policy document. Eur Arch Paediatr Dent 2022;23:3-21.ArticlePubMed
- 8. Shields S, Chen T, Crombie F, Manton DJ, Silva M. The impact of molar incisor hypomineralisation on children and adolescents: a narrative review. Healthcare (Basel) 2024;12:370.ArticlePubMedPMC
- 9. Brännström M. Sensitivity of dentine. Oral Surg Oral Med Oral Pathol 1966;21:517-526.ArticlePubMed
- 10. Dionysopoulos D, Gerasimidou O, Beltes C. Dentin hypersensitivity: etiology, diagnosis and contemporary therapeutic approaches: a review in literature. Appl Sci 2023;13:11632.Article
- 11. Ozen T, Orhan K, Avsever H, Tunca YM, Ulker AE, Akyol M. Dentin hypersensitivity: a randomized clinical comparison of three different agents in a short-term treatment period. Oper Dent 2009;34:392-398.ArticlePubMedPDF
- 12. Kim JW, Park JC. Dentin hypersensitivity and emerging concepts for treatments. J Oral Biosci 2017;59:211-217.Article
- 13. Greenwall-Cohen J, Greenwall L, Barry S. Silver diamine fluoride: an overview of the literature and current clinical techniques. Br Dent J 2020;228:831-838.ArticlePubMedPDF
- 14. Stebbins EA. What value has argenti nitras as a therapeutic agent in dentistry? Int Dent J (Phila) 1891;12:661-671.PubMedPMC
- 15. Peng JJ, Botelho MG, Matinlinna JP. Silver compounds used in dentistry for caries management: a review. J Dent 2012;40:531-541.ArticlePubMed
- 16. Cavalcante BG, Mlinkó É, Szabó B, Teutsch B, Hegyi P, Vág J, et al. Non-invasive strategies for remineralization and hypersensitivity management in molar-incisor hypomineralization: a systematic review and meta-analysis. J Clin Med 2024;13:7154.ArticlePubMedPMC
- 17. Erbas Unverdi G, Ballikaya E, Cehreli ZC. Clinical comparison of silver diamine fluoride (SDF) or silver-modified atraumatic restorative technique (SMART) on hypomineralised permanent molars with initial carious lesions: 3-year results of a prospective, randomised trial. J Dent 2024;147:105098.ArticlePubMed
- 18. Piovesan ÉT, Alves JB, Ribeiro CD, Massignan C, Bezerra AC, Leal SC. Is silver diamine fluoride effective in reducing dentin hypersensitivity?: a systematic review. J Dent Res Dent Clin Dent Prospects 2023;17:63-70.ArticlePubMedPMCPDF
- 19. Tricco AC, Lillie E, Zarin W, O'Brien KK, Colquhoun H, Levac D, et al. PRISMA Extension for Scoping Reviews (PRISMA-ScR): checklist and explanation. Ann Intern Med 2018;169:467-473.ArticlePubMed
- 20. Covidence systematic review software [Internet]. Melbourne: Veritas Health Innovation; 2025 [cited 2025 Mar 27]. Available from: https://www.covidence.org/
- 21. Al-Nerabieah Z, AlKhouli M, Dashash M. Preventive efficacy of 38% silver diamine fluoride and CPP-ACP fluoride varnish on molars affected by molar incisor hypomineralization in children: a randomized controlled trial. F1000Res 2024;12:1052.ArticlePubMedPDF
- 22. Saad AE, Alhosainy AY, Abdellatif AM. “Evaluation of Silver Diamine Fluoride Modified Atraumatic Restorative Treatment (SMART) on hypomineralized first permanent molar”: a randomized controlled clinical study. BMC Oral Health 2024;24:1182.ArticlePubMedPMCPDF
- 23. Ballikaya E, Ünverdi GE, Cehreli ZC. Management of initial carious lesions of hypomineralized molars (MIH) with silver diamine fluoride or silver-modified atraumatic restorative treatment (SMART): 1-year results of a prospective, randomized clinical trial. Clin Oral Investig 2022;26:2197-2205.ArticlePubMedPDF
- 24. Khan MK. Comprehensive management of molar-incisor-hypomineralization by preventive, palliative, and restorative treatment modalities in a pediatric patient: a case report and literature review. J Dent Res Rev 2022;9:173-179.ArticlePDF
- 25. Menzel M, Kiesow A, de Souza E Silva JM. Nano-CT characterization of dentinal tubule occlusion in SDF-treated dentin. Sci Rep 2023;13:15895.ArticlePubMedPMCPDF
- 26. Kiesow A, Menzel M, Lippert F, Tanzer JM, Milgrom P. Dentin tubule occlusion by a 38% silver diamine fluoride gel: an in vitro investigation. BDJ Open 2022;8:1.ArticlePubMedPMCPDF
- 27. Seto J, Horst JA, Parkinson DY, Frachella JC, DeRisi JL. Enhanced tooth structure via silver microwires following treatment with 38 percent silver diamine fluoride. Pediatr Dent 2020;42:226-231.PubMedPMC
- 28. Li Y, Liu Y, Psoter WJ, Nguyen OM, Bromage TG, Walters MA, et al. Assessment of the silver penetration and distribution in carious lesions of deciduous teeth treated with silver diamine fluoride. Caries Res 2019;53:431-440.ArticlePubMedPDF
- 29. Yoshiyama M, Masada J, Uchida A, Ishida H. Scanning electron microscopic characterization of sensitive vs. insensitive human radicular dentin. J Dent Res 1989;68:1498-1502.ArticlePubMedPDF
- 30. Seifo N, Robertson M, MacLean J, Blain K, Grosse S, Milne R, et al. The use of silver diamine fluoride (SDF) in dental practice. Br Dent J 2020;228:75-81.ArticlePubMedPDF
- 31. Garg S, Sadr A, Chan D. Potassium iodide reversal of silver diamine fluoride staining: a case report. Oper Dent 2019;44:221-226.ArticlePubMedPDF
- 32. Bal C, Sozuoz MA, Sari MB, Aksoy M. 1-year results of molar incisor hypomineralization-affected cases treated with silver modified atraumatic restorative treatment: a retrospective study. Int J Clin Pediatr Dent 2024;17:683-689.ArticlePubMedPMC
- 33. Ghanim A, Silva MJ, Elfrink ME, Lygidakis NA, Mariño RJ, Weerheijm KL, et al. Molar incisor hypomineralisation (MIH) training manual for clinical field surveys and practice. Eur Arch Paediatr Dent 2017;18:225-242.ArticlePubMedPDF
- 34. Jälevik B. Prevalence and diagnosis of molar-incisor- hypomineralisation (MIH): a systematic review. Eur Arch Paediatr Dent 2010;11:59-64.ArticlePubMedPDF
- 35. Jayanti CN, Riyanti E. Treatment alternative of molar incisor hypomineralisation for young permanent teeth: a scoping review. Clin Cosmet Investig Dent 2024;16:337-348.ArticlePubMedPMCPDF
REFERENCES
Tables & Figures
REFERENCES
Citations

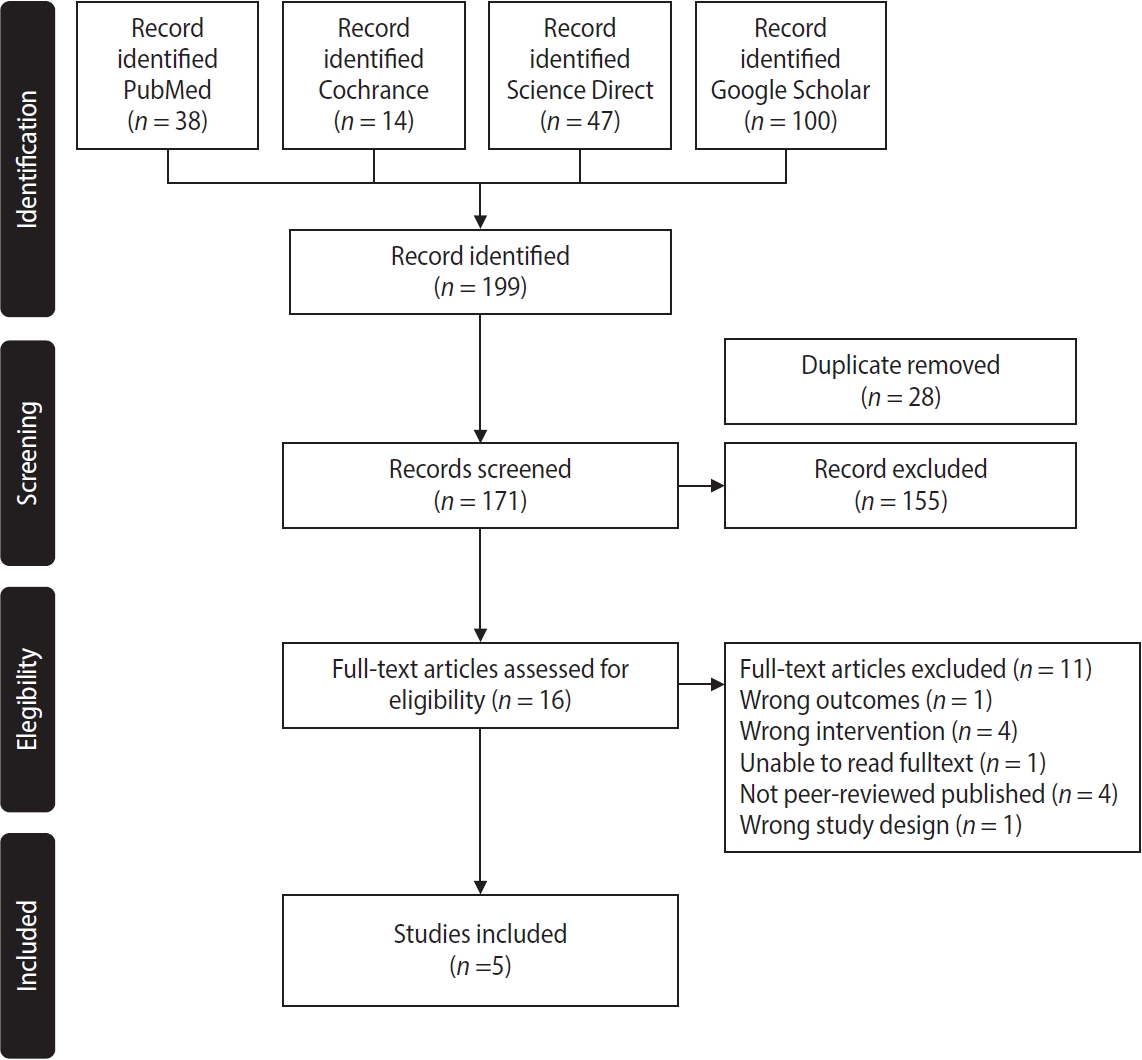
Figure 1.
| Database | Query |
|---|---|
| PubMed | ((((((sensitivity) OR (hypersensitivity)) OR (sensitive)) OR (dentin hypersensitivity)) OR (dentin sensitivity)) AND ((((((((SDF) OR (silver diamine fluoride)) OR (silver diammine fluoride)) OR (Ag(NH3)2F)) OR (diamine silver fluoride)) OR (conservative management)) OR (preventive approach)) OR (non-invasive strategies))) AND (((((((((MIH) OR (molar–incisor hypomineralisation)) OR (molar–incisor hypomineralization)) OR (molar–incisor-hypomineralisation)) OR (molar–incisor-hypomineralization)) OR (hypomineralisation)) OR (hypomineralization)) OR (hypomineralized enamel defect)) OR (hypomineralised enamel defect)) |
| The Cochrane Library | (sensitivity) OR (hypersensitivity) OR (sensitive) OR (dentin hypersensitivity) OR (dentin sensitivity) in Title Abstract Keyword AND (SDF) OR (silver diamine fluoride) OR (silver diammine fluoride) OR (Ag(NH3)2F) OR (diamine silver fluoride) OR (conservative management) OR (preventive approach) OR (non-invasive strategies) in Title Abstract Keyword AND (MIH) OR (molar–incisor hypomineralisation) OR (molar–incisor hypomineralization) OR (molar–incisor-hypomineralisation) OR (molar–incisor-hypomineralization) OR (hypomineralisation) OR (hypomineralization) OR (hypomineralized enamel defect) OR (hypomineralised enamel defect) in Title Abstract Keyword |
| ScienceDirect | (("sensitivity") OR ("sensitive") OR ("hypersensitivity")) AND (("silver diamine fluoride") OR ("SDF") OR ("non-invasive strategies")) AND ((“hypomineralization”) OR (“molar–incisor hypomineralization”)) |
| Google Scholar | (("sensitivity") OR ("sensitive") OR ("hypersensitivity")) AND (("silver diamine fluoride") OR ("SDF") OR ("non-invasive strategies")) AND ((“hypomineralization”) OR (“molar–incisor hypomineralization”)) |
| Inclusion criteria | Exclusion criteria |
|---|---|
| 1. Participants: children with at least one permanent molar clinically diagnosed with molar-incisor hypomineralization (MIH), with hypersensitivity symptoms, regardless of gender or geographic location. | 1. Non-human research: Studies involving in vitro, ex vivo, animal, cadaveric, or computational model-based designs. |
| 2. Intervention: application of silver diamine fluoride (SDF), either alone or in combination with other restorative or protective materials (e.g., SDF + potassium iodide, SMART technique, stainless steel crowns). | 2. Secondary or non-original literature: Review articles (systematic, scoping, or narrative), editorials, commentaries, letters to the editor, and other non–peer-reviewed or supplementary materials such as conference abstracts, examination documents, indices, tables of contents, book reviews, preview programs, or chart documentation. |
| 3. Outcomes: studies reporting quantitative or qualitative measures of dentin hypersensitivity, such as the Schiff cold air sensitivity scale, visual analog scale, or equivalent clinical sensitivity assessments. | 3. Irrelevant study scope: Articles that do not evaluate the effectiveness of SDF in the management of hypersensitivity in MIH-affected molars. |
| 4. Follow-up: any duration of follow-up, but the study must have included at least one post-treatment evaluation of hypersensitivity. | 4. Language and accessibility: Non-English publications or studies that are unable to be read in full-text versions. |
| 5. The study design can be observational (case-control, cohort, or other longitudinal) or experimental (randomized controlled trials, non-randomized controlled trials, or quasi-experimental), which published in peer-reviewed journals. | 5. Ethical or methodological deficiencies: Studies lacking ethical approval or adequate methodological description to confirm inclusion criteria. |
| No. | Study | Year | Research location | Research type | Sample (people) | Sample (molar) | Sex | Age (yr) | Research strategy | Tooth severity | Follow- up interval |
|---|---|---|---|---|---|---|---|---|---|---|---|
| 1 | Khan [24] | 2022 | India | Case report | 1 | 4 | Male | 8 | Evaluate the effect of SDF + stainless steel in reducing sensitivity on MIH-affected molars. | Severe | 3 mo |
| 2 | Ballikaya et al. [23] | 2022 | Türkiye | RCTs | 48 | 112 | Female, 30/male, 18 | 8.8 ± 1.58 | Evaluate and compare the effect of SDF and SMART sealants for the treatment of initial carious lesions of permanent molars affected by MIH. | NA | 1 mo, 6 mo, and 12 mo |
| 3 | Erbas Unverdi et al. [17] | 2024 | Türkiye | RCTs | 48 | 112 | Female, 30/male, 18 | 8.8 ± 1.58 | Assess the clinical outcomes of utilizing SDF + KI treatment and SMART/SDF + KI + GIC | NA | 12 mo, 18 mo, 24 mo, and 36 mo |
| 4 | Saad et al. [22] | 2024 | Egypt | RCTs | 28 | 56 | Female, 20/male, 8 | 6–10 | Compare SMART vs the conventional restoration and fluoride varnish application on moderate to severe MIH teeth | Moderate–severe | 1 wk, 6 mo, and 12 mo |
| 5 | Al-Nerabieah et al. [21] | 2024 | Syria | RCTs | 100 | 200 | NA | 6–9 | Compare the efficacy of SDF and CPP-ACPFV in preventing caries development, enamel breakdown, and sensitivity on molars affected by MIH in children. | Mild | 3 mo, 6 mo, 9 mo, and 12 mo |
| No. | Study | Treatment result | |||||
|---|---|---|---|---|---|---|---|
| SDF | SDF + KI | SMART/SDF + KI + GIC | SDF + stainless steel | CCP-ACPFV | Conventional restoration and fluoride varnish | ||
| 1 | Khan [24] | NA | NA | NA | SCASS scores deduce | NA | NA |
| 2 | Ballikaya et al. [23] | SCASS scores deduce | NA | SCASS scores deduce | NA | NA | NA |
| - Baseline: 1.77 ± 0.83 | - Baseline: 1.77 ± 0.83 | ||||||
| - 12th month: 0.15 ± 0.38 | - 12th month: 0.08 ± 0.28 | ||||||
| 3 | Erbas Unverdi et al. [17] | NA | SCASS scores deduce | SCASS scores deduce | NA | NA | NA |
| - SCASS scores = 0 (at the 18-month and beyond evaluations) | - SCASS scores = 0 (at the 18-month and beyond evaluations) | ||||||
| 4 | Saad et al. [22] | NA | NA | SCASS scores deduce | NA | NA | SCASS scores deduce |
| - Baseline: +MOD: 1.5/+ SEV: 3 | - Baseline: +MOD: 1.5/+SEV: 3 | ||||||
| - 12th month: +MOD: 0/+SEV: 0 | - 12th month: +MOD: 0/+SEV: 0 | ||||||
| 5 | Al-Nerabieah et al. [21] | SCASS scores deduce | NA | NA | NA | SCASS scores deduce | NA |
| No. | Study | Treatment result | |||||
|---|---|---|---|---|---|---|---|
| SDF | SDF + KI | SMART/SDF+KI+GIC | SDF + stainless steel | CCP-ACPFV | Conventional restoration and fluoride varnish | ||
| 1 | Khan [24] | NA | NA | NA | NA | NA | NA |
| 2 | Ballikaya et al. [23] | - No dental caries presented | NA | - No dental caries presented | NA | NA | NA |
| - Retention rate: NA | - Retention rate: 88.7% | ||||||
| 3 | Erbas Unverdi et al. [17] | NA | - The caries preventive effect was 100%, 67.9%, and 65.4% at 12, 24, and 36 months, respectively | - The caries preventive effect was 100%, 97.6%, and 94.7% at 12, 24, and 36 months, respectively | NA | NA | NA |
| - Retention rate: NA | - Retention rate: 88.7%, 73.1%, and 66.6% at 12, 24, and 36 months, respectively | ||||||
| 4 | Saad et al. [22] | NA | NA | - Caries prevention: NA | NA | NA | - Caries prevention: NA |
| - Restoration integrity | - Restoration integrity | ||||||
| +6th month: MOD: 1, SEV: 1 | +6th month: MOD: 1, SEV: 1 | ||||||
| +12th month: MOD: 1, SEV: 1 | +12th month: MOD: 1, SEV: 1 | ||||||
| 5 | Al-Nerabieah et al. [21] | - Caries rate was 11%, 15%, 21%, and 23% at 3, 6, 9, and 12 months, respectively | NA | NA | NA | - Caries rate was 33%, 39%, 44%, and 49% at 3, 6, 9, and 12 months, respectively | NA |
| - Retention rate: NA | - Retention rate: NA | ||||||
There were no limitations on time, sample size, or study location.
CPP-ACPFV, casein phosphopeptide-amorphous calcium phosphate fluoride varnish; GIC, glass ionomer cement; KI, potassium iodide; MIH, molar incisor hypomineralization; NA, not applicable; RCT, randomized clinical trial; SDF, silver diamine fluoride; SMART, silver-modified atraumatic restorative treatment.
CPP-ACPFV, casein phosphopeptide-amorphous calcium phosphate fluoride varnish; GIC, glass ionomer cement; KI, potassium iodide; MIH, molar incisor hypomineralization; MOD, moderate hypomineralized molar severity; NA, not applicable; SCASS, Schiff cold air sensitivity scale; SDF, silver diamine fluoride; SEV, severe hypomineralized molar severity; SMART, silver-modified atraumatic restorative treatment.
CPP-ACPFV, casein phosphopeptide-amorphous calcium phosphate fluoride varnish; GIC, glass ionomer cement; KI, potassium iodide; MIH, molar incisor hypomineralization; MOD, moderate hypomineralized molar severity; NA, not applicable; SDF, silver diamine fluoride; SEV, severe hypomineralized molar severity; SMART, silver-modified atraumatic restorative treatment.

 KACD
KACD
 Cite
Cite